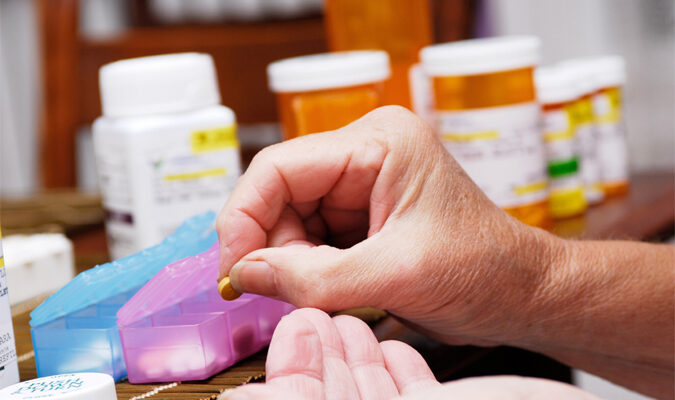
As we get older, our medication needs increase. Studies show that 23 percent of seniors have at least five items on their prescription list.
Staying on top of your medication management is crucial for your health. Physiological changes related to the aging process affect the way we absorb and metabolize drugs. Every medication regimen requires close monitoring and potential adjustments over time.
Despite that, many older adults neglect their medication. They forget about their doses, don’t take medicine as instructed, or stop taking it altogether. On top of that, having more than one prescribing physician can make it harder to track medicines.
The only real solution is to be proactive in managing your medication. Here are seven tips that should put you on the right track.
1. Consult With Your Doctor
Some medicines have side effects that cause dizziness or nausea. Others are more likely to cause falls or other accidents.
To prevent this from happening, go over your medicines with your doctor or pharmacist. If you’re taking a combination of medicines that could be dangerous, they’ll let you know about it. If you have any questions about your dosage, this is the right time to ask.
It’s best to keep repeating this process once a year. From time to time, you may need to reduce medication to a lower dose or switch to a safer alternative. If you’re experiencing unwanted side effects, head to your healthcare provider right away.
2. Use a Pillbox or Dispenser
The best way to keep track of your medication schedule is to use a pill organizer. Your two top options are a pillbox and an automatic dispenser.
Most pillboxes come with seven compartments for each day of the week. Others have 30 or 31 compartments, which can cover an entire month. By filling out your pillbox, you can keep your medication organized and refill it as needed.
Pillboxes come in many types, so choosing one can seem overwhelming. The main thing to focus on is ensuring that the compartments are large enough for your pills. If you’re still unsure, you can always ask your doctor or pharmacist for advice.
You can also invest in a dispenser, which dispenses your medication at a set time each day. Some models come with advanced features, such as tamper-proof locks. For example, MedReady Medication Management offers seven dispenser models for all needs.
3. Don’t Self-Medicate
Taking medication as prescribed can be of utmost importance to your health. The last thing you should do is think you know better than your doctor.
Many people tend to reduce or stop taking medication when they start feeling better. Though you may be on the right track, you shouldn’t do anything without speaking to your doctor first. Skipping your doses—even rarely—isn’t a good idea either.
On a similar note, you should never increase your dose frequency, even if you’re in pain. If you’re experiencing adverse reactions, talk to your doctor about adjusting your prescriptions. Do the same if you feel that your medication isn’t working.
4. Use a Single Pharmacy
After an appointment, it’s tempting to get your medicine from the nearest drugstore. More often than not, though, this won’t be your best option.
What you should do instead is get all your prescription refills at the same pharmacy if possible. That way, your pharmacist can help you keep track of your medication. If they notice any combinations of drugs that are a red flag, they can contact your doctor.
Going to one pharmacy also makes you more likely to get your prescriptions filled on time. It’s possible to transfer prescriptions between pharmacies, but some information may get lost. Among other things, this can cause delays in your refills.
5. Set Reminders
A pillbox or dispenser is a nice start, but it may not be enough. To ensure you stay on track, consider using a medication reminder system.
This can be as simple as setting a reminder on your smartphone. You can also use a multi-alarm clock, which is both inexpensive and easy to set up. Some devices targeted toward seniors allow you to program reminders throughout the day.
These devices are particularly useful for caregivers looking after older adults. They make mundane tasks a bit easier and allow caregivers to focus on more important things.
6. Store Medication Properly
Plenty of medications have specific storage instructions. Some should sit at a dry and cool temperature, whereas others need refrigeration.
If some of your medication comes with these instructions, keep it in the right place. For example, most bathrooms heat up and become humid after a shower. This causes the bathroom cabinet to let in extra moisture, which may impact the efficiency of the drug.
For this reason, it’s best to store your medication in your bedroom or living room. Make sure to keep your medication in its original packaging so you always know where it should go.
7. Read the Instructions Carefully
Speaking of medication instructions, make sure to read them thoroughly. For best results, go over them with your doctor or pharmacist.
Many instructions are specific about whether to take them with or without food and water. Some prevent you from drinking alcohol while you’re using them. If you forget about a dose, you may need to skip it if it’s too close to the next one.
On top of that, you must be aware of any dangerous food-drug interactions. For instance, leafy vegetables contain vitamin K, which can reduce the effectiveness of blood thinners. Another example is grapefruit, which can overcorrect blood pressure.
More on Medication Management
Medication management can seem scary, but organizing the more mundane tasks is a big help. The seven tips above are a good place to start.
The most important part of medication organization is making it a routine. If you’re not a fan of alarms, use a visual cue chart to develop your habits. Take colored pieces of paper that say which medicine to take when and put them on your bathroom mirror.
Looking for more ideas on how to organize your daily medication? Interested in building a bathroom cabinet that doesn’t let in moisture? Keep reading our medicine-related content!
Leave a Reply